Using virtual reality mobility testing as a standardized clinical end point in inherited retinal disorders
The use of VR mazes hold an intrinsic advantage compared with physical mazes in the ability to control conditions and test various patterns with reliability, participant safety, and repeatability.
The rise of the maze has been an attempt to evaluate the functional impact of a potential therapy. (Image Credit: ©Nikolai Sorokin - Adobe.Stock.com)

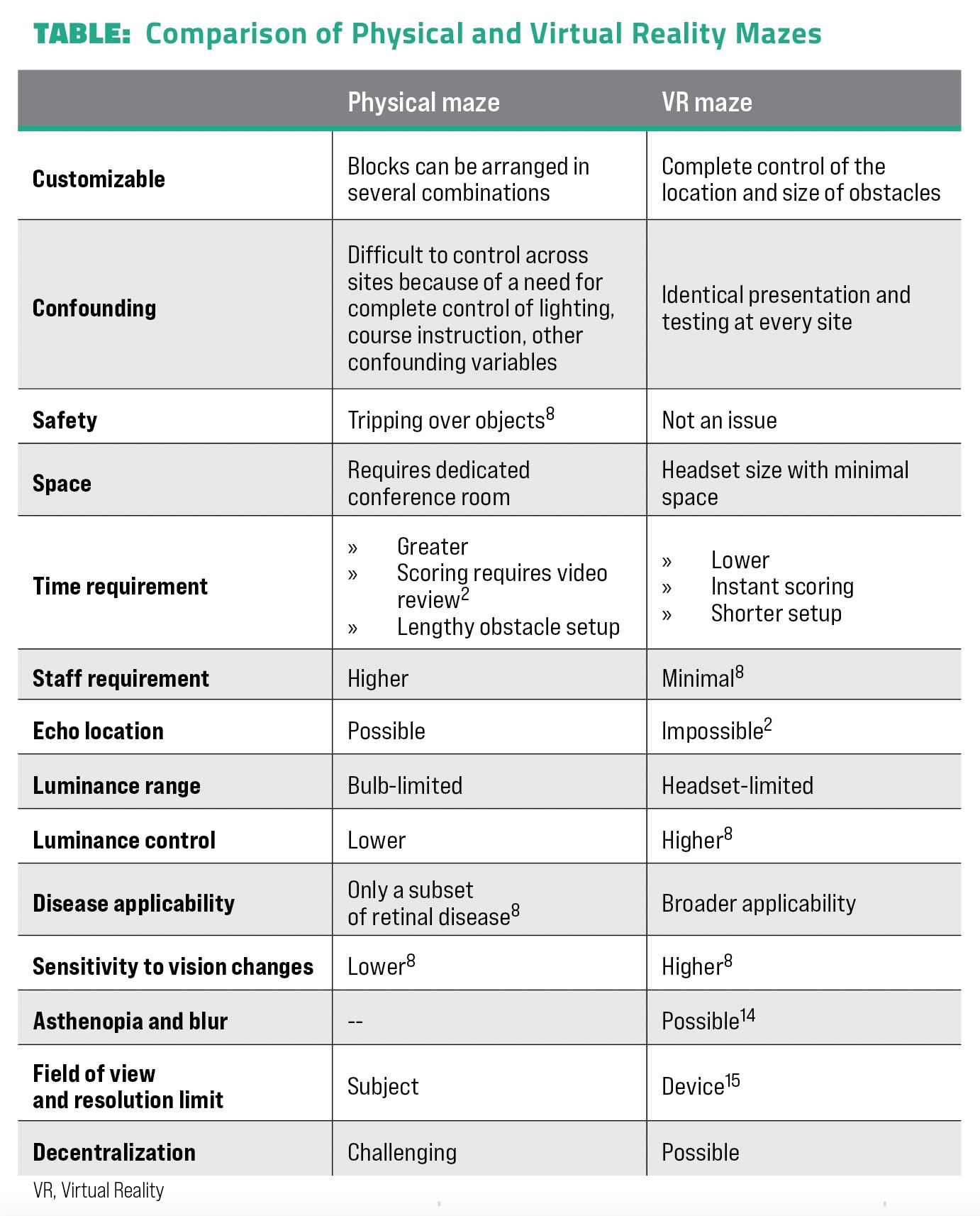
Mobility tests, which are sometimes also called mazes, were developed in the Luxturnaclinical trial and are common in inherited retinal disorder (IRD) clinical trials. The rise of the maze has been an attempt to evaluate the functional impact of a potential therapy. The recent development in virtual reality (VR) headset use creates a possibility that VR mobility assessments could become standard for clinical trial efficacy end points. For physical mazes, such as Chung et al’s multi-luminance mobility test (MLMT), patients might follow arrows, navigate steps, avoid obstacles, and identify a door at the end, with the ability to navigate measured at different luminance levels.1 Alternatively, in VR mazes, such as Aleman et al’s virtual reality mobility test, patients wear goggles, foot trackers, and hand trackers while following virtual arrows toward a virtual door (see Table for a comparison of VR and physical mazes).2 The use of VR mazes hold an intrinsic advantage compared with physical mazes in the ability to control conditions and test various patterns with reliability, participant safety, and repeatability.
The RUSH2A study was the largest and most well-controlled natural history study completed in patients with Usher disease. This study evaluated many functional and structural end points3:
- static rod and cone-mediated full-field
stimulus threshold (FST); - seeing area (kinetic perimetry);
- static perimetry total hill of vision;
- rod and cone mediated full-field
electroretinogram; - microperimetry assessment of mean retinal sensitivity;
- optical coherence tomography (OCT) assessment of ellipsoid zone area, central subfield thickness, evaluation for retinal cysts; and
- best corrected visual acuity.
While the RUSH2A end points will serve as a reference for IRD clinical trial end points, this study did not employ mobility testing, signaling a potential move away from a physical maze.
Recently, the FDA approved pegcetacoplan based on a structural end point, evaluation of geographic atrophy on fundus autofluorescent imaging.4,5 This approval was the first without a functional end point and signifies a potential opportunity in IRD trials to utilize structural end points, such as photoreceptor loss on OCT. Nevertheless, a functional test that translates into real-world activities could have added benefits, such as gauging patients’ ability to navigate streets or drive a vehicle. While Marron and Bailey previously tested patients’ mobility on a city block with obstacles of varying spatial detail and contrast, such a resource-intense test may not be universally feasible.6 However, mobility testing could serve as a functional end point in patients with nystagmus who cannot fixate on a perimetry target and thus cannot demonstrate a reliable structure-function end point.7 Bennett et al argue there is a need for a test that quantifies a patient’s ability to perceive their physical environment that incorporates numerous vision aspects necessary for activities of daily living, such as resolution, movement, and others.8
(Table content provided by article authors.)
Investigators have employed real-world mobility testing to evaluate IRDs. Russell et al employed the MLMT to assess voretigene neparvovec efficacy on IRD patients and found that treated patients performed significantly better than controls in low and moderate light.9 Chung et al used the same MLMT to evaluate mobility performance of control, retinitis pigmentosa (RP), Stargardt disease, choroideremia, Usher syndrome, and Leber congenital amaurosis (LCA) patients and found that only the LCA and RP patients demonstrated reduced performance over 1 year, and that the test distinguished between controls and disease patients.1 Similarly, Roman et al tested LCA patients with GUCY2D and CEP290 mutations, found a linear relationship between mobility and FST, and report that their findings can be used to quantify clinical trial outcomes.7 Additionally, Kumaran et al validated a physical vision-guided mobility test for patients with RPE65-mediated IRD and found that mobility correlated to perimetry and can serve as a resource for future interventions.10 Furthermore, investigators used physical mazes to assess the efficacy of botaretigene sparoparvovec in patients with x-linked RP and found, at 26 weeks, the low- and intermediate-dose–treated patients improved visual mobility maze performance relative to untreated patients.11 In 1 patient’s case, visual mobility maze performance improved from 61.7 seconds at baseline to 16.4 seconds 9 months after therapy.12
Investigators also use VR to assess IRD patient mobility. Aleman et al used VR with a maze similar to Chung et al’s maze to assess patients with RPE65-associated LCA before and after voretigene neparvovec therapy and found treated patients improved in speed, accuracy, and illumination requirement.2 Further, before therapy, patients required guide assistance to navigate dim
sidewalks and hallways, but after therapy did so independently, accurately, and successfully. Thus, Aleman et al makes a case that VR does correspond with the “real world.”2 Bennett et al used a VR system to show that their VR protocol distinguishes between IRD and normally sighted patients, and that IRD patients require greater brightness to complete orientation and mobility testing.8 Bennett et al’s protocol could distinguish eyes in asymmetric disease presentation, suggesting it could assess patients undergoing monocular therapy in clinical trials.8
Chebat et al evaluated sighted, blindfolded, low vision and late blind, and congenitally blind subjects in physical and virtual mazes and found that low vision and late blind subjects made significantly higher real-maze collisions relative to other groups.13 Collisions are concerning and, thus, VR mazes demonstrate the advantages noted in Table.
VR mazes are safer, more practical, and offer greater variability. Alternatively, physical mazes better replicate the real world. Given that few sites have the space to support physical mazes, the industry should look closely at VR opportunities. If the industry adopts standardized mobility assessments into clinical trials, they will need to attain a series of milestones.
First, a comparison of VR and physical mobility tests is necessary. While voretigene neparvovec received FDA approval via a mobility test, a thorough comparison of performance of a physical mobility assessment and VR assessment in the same population is necessary to determine that a VR maze is also a valid assessment of IRD. Second, the ophthalmology community will likely need to determine a standardized test. Once determined, the professional organizations might consider refining their preferred practice patterns to include IRDs and specify mobility testing as diagnostic and ancillary tests.16 Third, the FDA should refine its guidance regarding human gene therapy for retinal disorders to specify preferred mobility tests parameters for clinical end points; currently the FDA suggests it is open to collaborating on end points.17 Importantly, the MLMT test was reportedly critical to voretigene neparvovec’s FDA approval, which suggests future clinical trials should consider mobility testing.18 As clinical trials for IRDs become prevalent, the FDA has a limit on resources it can allocate toward any one venture. With specific and standardized FDA IRD end point guidance, the ophthalmology community may be encouraged to pursue a greater number of IRD trials without any delays because of FDA coordination.
The views expressed in this article are those of the authors and do not reflect the official policy or position of the Department of the Army, Department of Defense, or the US Government.
REFERENCES
Chung DC, McCague S, Yu ZF, et al. Novel mobility test to assess functional vision in patients with inherited retinal dystrophies. Clin Exp Ophthalmol. 2018;46(3):247-259. doi:10.1111/ceo.13022
Aleman TS, Miller AJ, Maguire KH, et al. A virtual reality orientation and mobility test for inherited retinal degenerations: testing a proof-of-concept after gene therapy. Clin Ophthalmol. 2021;15:939-952. doi:10.2147/OPTH.S292527
Duncan JL, Liang W, Maguire MG, et al. Baseline visual field findings in the RUSH2A study: associated factors and correlation with other measures of disease severity. Am J Ophthalmol. 2020;219:87-100. doi:10.1016/j.ajo.2020.05.024
Chambers W. FDA. February 17, 2023. Accessed June 15, 2023. https://www.accessdata.fda.gov/drugsatfda_docs/appletter/2023/217171Orig1s000ltr.pdf
Goldberg R, Heier JS, Wykoff CC, et al. Efficacy of intravitreal pegcetacoplan in patients with geographic atrophy (GA): 12-month results from the phase 3 OAKS and DERBY studies. Invest Ophthalmol Vis Sci. 2022;63(7):1500.
Marron JA, Bailey IL. Visual factors and orientation-mobility performance. Am J Optom Physiol Opt. 1982;59(5):413-426. doi:10.1097/00006324-198205000-00009
Roman AJ, Cideciyan AV, Wu V, et al. Mobility test to assess functional vision in dark-adapted patients with Leber congenital amaurosis. BMC Ophthalmol. 2022;22(1):266. doi:10.1186/s12886-022-02475-y
Bennett J, Aleman EM, Maguire KH, et al. Optimization and validation of a virtual reality orientation and mobility test for inherited retinal degenerations.Transl Vis Sci Technol. 2023;12(1):28. doi:10.1186/s12886-022-02475-y
Russell S, Bennett J, Wellman JA, et al. Efficacy and safety of voretigene neparvovec (AAV2-hRPE65v2) in patients with RPE65-mediated inherited retinal dystrophy: a randomised, controlled, open-label, phase 3 trial. Lancet. 2017;390(10097):849-860. doi:10.1016/S0140-6736(17)31868-8
Kumaran N, Ali RR, Tyler NA, Bainbridge JWB, Michaelides M, Rubin GS. Validation of a vision-guided mobility assessment for RPE65-associated retinal dystrophy. Transl Vis Sci Technol. 2020;9(10):5. doi:10.1167/tvst.9.10.5
Janssen announces late-breaking data from two gene therapy programs at the American Academy of Ophthalmology 2022 Annual Meeting. News release. Johnson & Johnson. October 1, 2022. Accessed June 15, 2023. https://www.jnj.com/janssen-announces-late-breaking-data-from-two-gene-therapy-programs-at-the-american-academy-of-ophthalmology-2022-annual-meeting
Retinitis pigmentosa responds to gene therapy. American Academy of Ophthalmology. October 2, 2022. Accessed July 3, 2023. https://www.aao.org/eyenet/academy-live/detail/retinitis-pigmentosa-responds-to-gene-therapy
Chebat DR, Maidenbaum S, Amedi A. Navigation using sensory substitution in real and virtual mazes. PLoS ONE. 2015;10(6). doi:10.1371/journal.pone.0126307
Sheedy J, Bergstrom N. Performance and comfort on near-eye computer displays. Optom Vis Sci. 2002;79(5):306. doi:10.1097/00006324-200205000-00010
Lynn MH, Luo G, Tomasi M, Pundlik S, E. Houston K. Measuring virtual reality headset resolution and field of view: implications for vision care applications. Optom Vis Sci. 2020;97(8):573. doi:10.1097/OPX.0000000000001541
Retina summary benchmarks - 2022. American Academy of Ophthalmology. December 1, 2022. Accessed July 3, 2023. https://www.aao.org/education/summary-benchmark-detail/retina-summary-benchmarks-2020
Human gene therapy for retinal disorders: guidance for industry. January 2020. Accessed July 19, 2023.https://www.fda.gov/regulatory-information/search-fda-guidance-documents/human-gene-therapy-retinal-disorders
FDA media briefing on the first gene therapy approved in the U.S. to target a disease caused by mutations in a specific gene. FDA. December 19, 2017. Accessed July 19, 2023. https://www.fda.gov/media/109952/download

Newsletter
Keep your retina practice on the forefront—subscribe for expert analysis and emerging trends in retinal disease management.