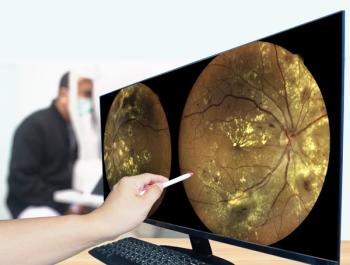
Central subfield thickness only partially responsible for changes in acuity
A post-hoc analysis of Protocol T from the
In phase III clinical studies evaluating anti-VEGF factors, VA is typically the primary outcome, but studies also use OCT CST measures as a secondary outcome. Some publications have reported that CST is the preferred OCT measurement for the central macula in DME because of its higher reproducibility and correlation with other measurements of the central macula.
The DRCR Retina Network’s trials use an algorithm based on changed in either vision or OCT to determine whether or not treatment is warranted after the initial 4-6 monthly injections. The group wrote that it seems reasonable “to use OCT CST changes as a surrogate for VA changes in DME because the objective determination of OCT CST is faster to obtain and less prone to subjective aspects of VA measurement.”
However, in Protocol I, where eyes were treated with focal/grid laser for DME, anatomic outcomes as determined by OCT CST only correlated moderately with VA. And in Protocol T (which randomly assigned 660 eyes to one of the three anti-VEGF agents), eyes that had less than 10% or more than a 20% change in CST reduction showed little difference in the percentage of eyes that gained 10 or more letters by year 2, regardless of anti-VEGF treatment.
“Furthermore, after 6 monthly injections of anti–VEGF therapy with 1 of these 3 agents, changes in VA between baseline and 2 years among eyes with persistent DME based on OCT CST were similar to changes in VA among eyes without persistent DME based on OCT CST,” the group wrote. In this post-hoc analysis, all eyes with complete VA and OCT CST measurements were included (n = 652).
CST accounted for 13% of the total variation in VA observed. The association between VA and CST was similar (3.3 letters; 95%CI, 2.7-3.9 letters) after accounting for the A1c level, which was the only other previously identified baseline variable significantly related to VA.
Overall, changes in CST accounted only for a small proportion (12%-14%) of the total variation in changes in VA at each follow-up visit. Yet for any given change in VA from baseline at 12, 52, and 104 weeks, there was a broad range of changes in OCT CST from baseline. The data suggested that the correlation coefficients of change in VA vs change in OCT CST at 12 weeks were greater when the baseline CST was 650 μm or more compared with greater than 350μmbut less than 450μm.
The findings of this post-hoc analysis were similar to those observed when laser treatment was used to treat DME, as in Protocol I. Further, the results are also consistent with findings after using anti-VEGFs to treat age-related macular degeneration.
“Thus, the preponderance of data to date suggests that one should not use change in OCT CST over time as a definitive surrogate for VA changes over time,” the study authors wrote. They did add, however, that because there is a general correlation between changes in OCT CST and changes in VA, using those changes as a surrogate outcomes for earlier phase clinical studies “seems reasonable.”
References:
1. Bressler NM, Odia I, Maguire M, et al. Association Between Change in Visual Acuity and Change in Central Subfield Thickness During Treatment of Diabetic Macular Edema in Participants Randomized to Aflibercept, Bevacizumab, or Ranibizumab: A Post Hoc Analysis of the Protocol T Randomized Clinical Trial. JAMA Ophthalmol 2019;137(9):977-85.