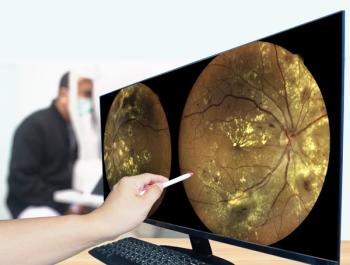
Up-to-the-minute diabetic updates for your patients
From the latest ADA position statements to special issues to dietary intake, here’s the latest info to share with your patients about diabetic eye disease.
The International Journal of Molecular Sciences is planning a special issue devoted to diabetic retinopathy, with a deadline for manuscript submissions of 24 Feb. 2019. (The first round closed in October 2018; papers published from that round are available online.) Peter Koulen, MD, of the University of Missouri-Kansas City, will serve as the special issue editor.
The journal notes that “with the ultimate goal to generate intervention strategies that slow or even reverse structural and functional degeneration of the retina and that attenuate or eliminate vascular complications input from numerous fields, such as neurology, ophthalmology, and endocrinology appears critically needed as effective therapies for DR are lacking.”
While acknowledging that methodological advances in synthetic and medicinal chemistry, mass spectrometry, proteomics, drug target discovery and drug development have generated significant developments in this field, more must be done.
“Therefore, this Special Issue invites manuscript submissions, namely research and review papers, targeting the gamut of methodological and scientific innovation in this field. Of specific interest to this special issue are papers focused on the discovery and mechanistic characterization of novel drug targets, signaling pathways, and mechanisms of action as they are relevant for DR. These contributions can be general and broad in their basic science and translational research focus or highly focused on specific research models related to structural and functional degeneration of the retina and vascular complications.”
There is an article processing charge of CHF1800 (about $1,800).
Systematic Review on Dietary Intake and DR
A systematic review published earlier this year1 identified nearly 4,300 studies using standardized criteria for diet and DR. The authors said that the reason for their analysis was that there is growing evidence linking dietary intake to DR, but nothing conclusive. Of those initial studies, the authors narrowed it down to three interventional and 28 observational studies.
Higher intakes of dietary fibre, oily fish, and greater adherence to a Mediterranean diet were protective of DR. Conversely, high total caloric intake was associated with higher risk of DR. No significant associations of carbohydrate, vitamin D, and sodium intake with DR were found. Associations of antioxidants, fatty acids, proteins and alcohol with DR remain equivocal.
They concluded that longitudinal data and interventional models are warranted to confirm our findings and better inform clinical guidelines.
High prevalence, high unawareness
A group of Indian researchers assessed the awareness of DR and its association with multiple comorbidities in a group of Indian patients, and found a high prevalence and significantly high unawareness for DR in patients with Type 2 diabetes.2
Unawareness also existed among the patients regarding the fact whether DR can be prevented or treated. The majority of patients reported to have undergone first dilated fundus examination only when their vision was affected. In this group of patients, the prevalence of retinopathy was 65%, nearly 3 times higher than other published studies of people in the same region.
Overall 6000 T2DM patients over 2 years were retrospectively evaluated. Almost 63% (n = 3780) of patients were unaware that diabetes affects the retina. Overall 52.02% (n = 1820) of smokers were reported of DR (P<0.00001). With the increase in total cholesterol and triglycerides, there was a significant increase in DR incidence (P<0.00001).
A strong association was observed between hypertension and DR, with 42.6% (n=2556) of patients having coexistence of hypertension and DR (P<0.00001). Patients having diabetic kidney disease also reported DR. A high proportion of patients (49.11%, n=2947) had co-existence of cardiac morbidity and DR. Almost 47% (n=2845) of patients having DR were also reported anemia. Totally 43.85% (n=2631) of patients with microalbuminuria had two times more risk of developing proliferative DR (P < 0.00001).
However, men were more affected with DR compared to women, which supports other large cohort findings.
ADA’s Position Statement
The American Diabetes Association’s position statements on DR have been published since 2002, but since that time, improvements in medications and devices for the systemic therapy of diabetes have also improved the ability of patients to optimize their metabolic control. The ADA’s latest position statement3 incorporates those developments. The ADA paper noted glaucoma, cataracts, and other disorders of the eye occur earlier and more frequently in people with diabetes.
Here are the key highlights from the group’s 2017 paper:
Natural history
- Optimize glycemic control to reduce the risk or slow the progression of DR.
- Optimize blood pressure and serum lipid control to reduce the risk or slow the progression of DR.
Screening Recommendations
- Adults with type 1 diabetes should have an initial dilated and comprehensive eye examination by an ophthalmologist or optometrist within 5 years after the onset of diabetes.
- Patients with type 2 diabetes should have an initial dilated and comprehensive eye examination by an ophthalmologist or optometrist at the time of the diabetes diagnosis.
- If there is no evidence of retinopathy for one or more annual eye exams, then exams every 2 years may be considered. If any level of DR is present, subsequent dilated retinal examinations for patients with type 1 or type 2 diabetes should be repeated at least annually by an ophthalmologist or optometrist. If retinopathy is progressing or sight-threatening, then examinations will be required more frequently.
- Women with preexisting type 1 or type 2 diabetes who are planning pregnancy or who have become pregnant should be counseled on the risk of development and/or progression of DR.
- Eye examinations should occur before pregnancy or in the first trimester in patients with preexisting type 1 or type 2 diabetes, and then these patients should be monitored every trimester and for 1 year postpartum as indicated by the degree of retinopathy.
- While retinal photography may serve as a screening tool for retinopathy, it is not a substitute for a comprehensive eye exam, which should be performed at least initially and at intervals thereafter as recommended by an eye care professional.
Treatment Recommendations
- Promptly refer patients with any level of macular edema, severe nonproliferative DR (NPDR, a precursor of proliferative DR), or any proliferative DR (PDR) to an ophthalmologist who is knowledgeable and experienced in the management and treatment of DR.
- Laser photocoagulation therapy reduces the risk of vision loss in patients with high-risk proliferative DR and, in some cases, severe nonproliferative DR.
- Intravitreous injections of anti–vascular endothelial growth factor are indicated for central-involved diabetic macular edema, which occurs beneath the foveal center and may threaten reading vision.
- The presence of retinopathy is not a contraindication to aspirin therapy for cardio protection, as aspirin does not increase the risk of retinal hemorrhage.
Raising awareness
Diopsys (Pine Brook, NJ) has noted the American Diabetes Association (ADA) released new research earlier this year estimating the total U.S. cost of diagnosed diabetes rose to $327 billion in 2017.
Recognizing the signs of DR on clinical examination or with imaging, however, is challenging, and many cases are identified only after permanent damage has occurred. Diopsys provides two different vision tests that can help eye care specialists detect and manage the disease earlier, and is using its platforms to also raise awareness of DR and the sight-threatening complications of diabetes.
The Diopsys Chromatic Flash Vision Screener is an in-office screening test and the company’s ffERG/Flicker testing protocols record the retina’s response to flashes of light to provide objective, functional information about global retinal health.
References:
1. Wong MYZ, Man REK, Fenwick EK, et al. Dietary intake and diabetic retinopathy: A systematic review. PLOSOne. Doi:10.1371/journal.pone.0186582
2. Shah K, Gandhi A, Natarajan S. Diabetic retinopathy awareness and association with multiple comorbidities: Insights from DIAMOND study. Indian J Endocrinol Metab. 2018;22(1):30-35
3. Solomon SD, Chew E, Duh EJ, et al. Diabetic Retinopathy: A position statement by the American Diabetes Association. Diabetes Care. 2017;40:412-418. DOI: 10,2337/dc16-2641.
Newsletter
Keep your retina practice on the forefront—subscribe for expert analysis and emerging trends in retinal disease management.