Patient assistance programs can ease DME financial burden
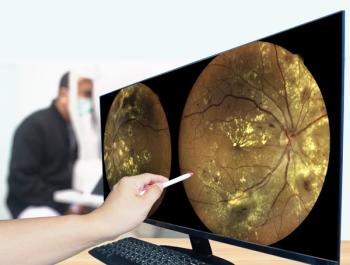
About 33% of patients with diabetes have diabetic retinopathy (DR), and, of those, 7% will progress to diabetic macular edema (DME).1 Patients with DR and/or DME incur significant medical costs.
One study found that patients with DME incurred between $20,166 and $29,959 in annual inpatient, outpatient, and pharmaceutical expenses.2 Those costs were even higher in DME patients with vision impairment, ranging between $27,574 and $42,692. DME cost the United States around $5.35 billion in 2007 alone.
Anecdotally, it is not uncommon to hear of patients who miss appointments or become lost to follow-up at retinal clinics while other complications of their systemic disease take precedence.
Because of the significant financial burden that patients with DR and/or DME experience, a number of pharmaceutical companies have created patient assistance programs to help alleviate the economic burden:
- Allergan Retina, for example, has a patient assistance program for Ozurdex (dexamethasone intravitreal implant), which is used in the management of recalcitrant DME. The program helps uninsured and underinsured patients who may not otherwise be able to afford Ozurdex. Patients can enroll in their doctor’s office if eligible.
- Genentech has a number of options to help patients pay for ranibizumab (Lucentis) through its Lucentis Access Solutions program. Lucentis Access Solutions will help patients calculate their expected co-pay and refer patients with public and commercial insurance to independent co-pay assistance foundations. Lucentis Access Solutions offers referrals to the Genentech Patient Foundation, which provides free Genentech medications to patients who don’t have insurance, whose treatment is not covered by insurance, or who are unable to pay the out-of-pocket expenses.
Lucentis Access Solutions also refers patients to the Lucentis Co-Pay Program, which helps patients cover out-of-pocket costs. Patients on Medicare, Medicaid, or other government insurance are not eligible for the program. Patients are encouraged to work with their physician on enrolling into the Lucentis Access Solutions program.
• Regeneron Pharmaceuticals offers patient assistance for aflibercept (Eylea) injections through its EYLEA4U program. Patients on commercial insurance may be eligible for assistance with co-pays, and patients on Medicare or Medicare Advantage can be referred to an independent co-pay assistance foundation. An EYLEA4U support specialist will discuss the different foundation options with patients, help patients apply to the foundation of their choice, and follow up with the foundation until a decision has been made on the application.
Patients with commercial insurance are offered the Eylea Injection Co-Pay Card Program, which covers up to $10,000 per year toward co-pays, co-insurance, and insurance deductibles for aflibercept injection treatments. Eligible patients pay the first $5 of each aflibercept treatment and any additional costs that exceed the $10,000 annual limit. It’s important to note that the program does not cover supplies, procedures, or physician-related expenses associated with Eylea.
EYLEA4U also offers financial aid for uninsured and underinsured patients and may be able to provide these patients with Eylea free of charge. To qualify, patients must be a resident of the United States and show financial need based on a total household income not exceed $100,000 per year.
• Alimera Sciences offers financial assistance for the fluocinolone acetonide intravitreal implant (Iluvien) through its AccessPlus program. Like Genentech and Regeneron, Alimera offers patients a Co-Pay Program that provides financial assistance for commercially insured patients with out-of-pocket expenses that exceed $25. Patients must be U.S. resident and not on a government insurance program. Patients who are accepted into the program will pay up to $25 per Iluvien injection. Patients on Medicare and Medicare Advantage will be referred to an independent co-pay foundation. AccessPlus support staff will help patients find foundations that are right for them and guide them through the application process.
Alimera Sciences also offers Iluvien free of charge for uninsured patients. To be eligible, patients must be a U.S resident, have no insurance or an insurance plan that won’t pay for the medication, and have a household income less than 500% of the Federal Poverty Limit. Patients will be asked to provide financial documentation.
Patients with DR and/or DME face significant life-long challenges including potential blindness, but may not be aware of the financial help available to them to ensure compliance with their treatments.
References:
1. Yau JW, Rogers SL, Kawasaki R, et al. Global prevalence and major risk factors of diabetic retinopathy. Diabetes Care. 2012;35:556-564.
2. Lanzetta P, Nuys KV, Tran I, et al. The Economic Burden of Diabetic Macular Edema from a U.S. Private Payer Perspective. Investigative Ophthalmology & Visual Science. 2011;52:5532.
Newsletter
Keep your retina practice on the forefront—subscribe for expert analysis and emerging trends in retinal disease management.