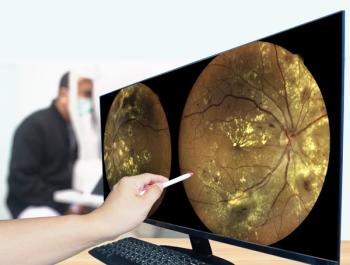
Guidelines for treating the diabetic eye patient
The most consistent means to lower the risk of developing complications from diabetes is for people to maintain good glycemic control. The new current criteria for the diagnosis of diabetes now includes two abnormal test results from the same sample (fasting plasma glucose and A1C from the same sample).
The most consistent means to lower the risk of developing complications from
The
That may be an issue, as the
Beyond just a yearly eye exam, referral to an ophthalmologist is required when there is any nonproliferative DR (NPDR), proliferative retinopathy (PDR), or macular edema. AAO also notes that at this point, laser photocoagulation remains the preferred treatment for non-center-involving DME.1 The
The
Based on those rates, somewhere around 100-200 million people have DR and possibly as many as 20-30 million have PDR or DME. More than 3 decades’ worth of landmark randomized clinical trials have shown the overwhelming majority (98%) of blindness could be prevented by either laser photocoagulation therapy or vitrectomy, and more recently, by the introduction of
“These treatments, coupled with the concept of earlier detection and systemic management of DM, such as intensive glucose and blood pressure control, have led to observations of declining rates of vision loss resulting from DR in the United States, Western Europe, and many countries over time,” the ICO wrote.4
By increasing public knowledge with targeted health care education; by creating well-implemented community-level or national screening programs for all persons with DM; increasing timely referral for more severe levels of DR; and finally, ensuring appropriate treatment for advanced DR such as PDR and DME, the public health perspective can be improved. But in many countries, a standard care pathway for DR management is not always clear.
Countries with high resources tend to have evidence-based guidelines, but “few comprehensive guidelines are available in low- or intermediate-resource countries.”
For example, only 11 of 50 Asian countries have some form of guidelines and of those, only two are specific to DR.4
The current ICO guidelines suggest the minimum screening examination components to ensure appropriate referral should include a screening vision examination (before pupil dilation if this is necessary) and a retinal examination adequate for DR classification. This can vary depending on high-resources settings or low- or intermediate resources settings. The vision exams can be completed by general practitioners, nurses, and healthcare works in community settings, the group said.
The screening program for DR “must be coupled with access to adequate and timely referral for ophthalmologic care.
The guidelines suggest that without appropriate and timely access to ophthalmologic care, screening patients with positive results will have no benefit from the DR screening program. Thus, DR screening programs should be started only after ensuring appropriate access to facilities with access to minimum treatment, including the availability of a laser machine and typically within 3 months of screening.”4
In terms of management, the ICO said panretinal photocoagulation (PRP) should be considered “the preferred choice of treatment of severe nonproliferative DR and all stages of PDR,” with the contemporary approach using short-pulse 20- to 30-ms laser with 2000 to 4000 treatment burns depending on the PDR grade and severity.
Patients with non-center involving DME may be observed until there is progression to central involvement, or focal laser can be performed to treat leaking microaneurysms if DME is threatening the fovea.4
Finally, the ICO said where the patient seeks treatment with center-involving DME and good visual acuity (better than 6/9 or 20/30), 3 treatment options are possible and are currently being evaluated in an ongoing clinical trial: (1) careful follow-up with anti-VEGF treatment only for worsening DME; (2) intravitreal anti-VEGF injections; or (3) focal or grid laser photocoagulation with anti-VEGF, if necessary.4
References:
1. American Academy of Ophthalmology Retina Panel. Preferred Practice Pattern: Diabetic Retinopathy. San Francisco, CA: AAO, 2016.
2. Summary of Revisions: Standards of Medical Care in Diabetes-2019. Diabetes Care. 2019;42(Suppl 1):S4-S6.
3. American Optometric Association. Eye Care of the Patient with Diabetes Mellitus: Evidence-Based Clinical Practice Guideline. Optometric Clinical Practice Guideline. Available from:
4. Wong TY, Sun J, Kawasaki R, et al. Guidelines on Diabetic Eye Care: The International Council of Ophthalmology Recommendations for Screening, Follow-up, Referral, and Treatment Based on Resource Settings. Ophthalmology. 2018;125:1608-1622.
Newsletter
Keep your retina practice on the forefront—subscribe for expert analysis and emerging trends in retinal disease management.